Renal anaemia is a normochromic normocytic anaemia (normal sized red cells with normal Hb content) that increases in severity as GFR falls. There are a number of explanations for renal anaemia, but relative deficiency of erythropoietin is usually dominant. However many patients require more than physiological doses of erythropoietin. Causes include:
- Erythropoietin deficiency
- Reduced RBC lifespan
- Disordered iron utilisation
- Blood loss in patients on dialysis
- Inflammation – anaemia of chronic disease
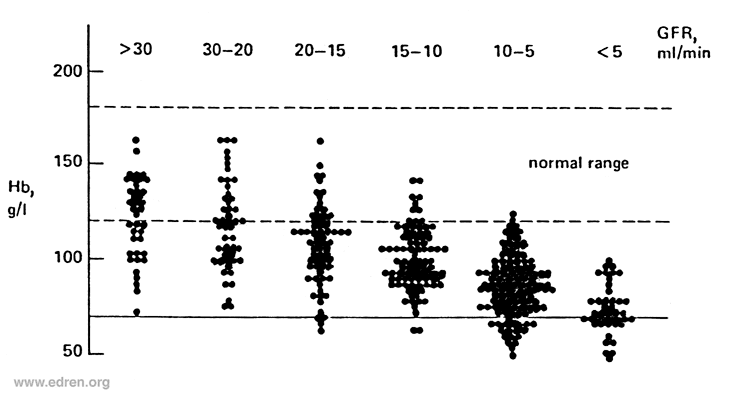
As the graph shows, without effective treatments anaemia can be very severe. The lowest haemoglobins are found in patients who have had their native kidneys removed, and the highest in those with big kidneys – e.g. polycystic kidneys. Blood transfusions risk iron overload and sensitisation to transplantation antigens, and before other effective treatments were available could only be used to prevent the most severe symptoms.
Management of renal anaemia
First look for other or contributing causes including deficiency of iron, folate etc. Then …
Erythropoietin – is a glycosylated hormone produced mostly by the kidney in response to reductions in oxygen delivery, such as occur as in anaemia, or in living at high altitude. The natural molecule is small enough for glomerular filtration to be a significant route of clearance, and traces of EPO can be found in normal urine.
The availability of different EPO-type drugs means these are now more properly called ‘erythropoiesis stimulating agents’, ESAs. EPO-like drugs may be closely similar to native EPO (but not identical, as some athletes have found out to their cost) or engineered to be bigger and so have longer half lives and some other properties. So far all require injection, from 2-3 times weekly to injections one or several weeks apart for the larger molecules. Blood pressure can rise as Hb rises. Development of EPO-neutralising antibodies to cause pure red cell aplasia (PRCA) is a very rare but serious complication of treatment with ESAs.
Iron management – Oral iron is poorly absorbed and utilised in patients with renal failure and periodic intravenous treatment is generally required. Higher ferritin values than usual are necessary to maximise erythropoiesis.
What target haemoglobin?
Patients feel better and can do more with a higher haemoglobin, and patients with lower haemoglobins seem to have higher mortality. So you might assume that restoring Hb to the normal range is best practice. Randomised trials have not supported that and have even suggested extra risk from returning Hb to the normal range versus slightly lower targets of 10-11g/dl (100-110g/l). There are two chief hypotheses to explain this:
- Higher Hb values predispose to thrombosis – renal patients have a higher risk of cardiovascular disease so do better with lower Hb values. Against this, excess morbidity and mortality observed hasn’t all been cardiovascular.
- The higher (supraphysiological) values of EPO required to generate normal Hb levels act on EPO receptors on other cells in addition to bone marrow cells, and produce some undesirable effects.