Contents
Dialysis patients/osteodystrophy
There is no need for any routine screening. Where hyperparathyroidism is being quantitated, a hand XR alone will usually suffice (request ‘hand XR for hyperparathyroidism’ in Edinburgh). Views of the pelvis may be justified in some circumstances – explain these on the request form if so.
Renal Arteriography and Angioplasty
MR and CT Angiography have greatly reduced use of conventional angiography. However concerns about Gadolinium-containing MR contrast media and Nephrogenic Systemic Fibrosis (Nephrogenic Sclerosing Dermopathy) mean that MRA be used very cautiously if at all in dialysis patients and patients with severe renal failure.
For conventional angiography, patients admitted on day of procedure, earlier if less fit. Overnight stay not routinely required for diagnostic angiograms, usually suitable for day case unit. Should stay overnight for interventions.
Pre-Procedure
- Warfarin – stop 3 days in advance and check clotting on morning of procedure
- Non-steroidals other than aspirin : stop on day of procedure and for 48h
- Metformin – omit on day of procedure and withhold for 48 hours, restart if function OK
- All other medications including anti-hypertensive and anti-anginal to continue
- Fluids only for 2 hours prior to procedure (can have light breakfast if late am procedure)
Investigations: recent results to be available for
- FBC (Hb must be >80g/l, Pts >100)
- U&E (K should be <5, if not give IV 10% dextrose 20mls/hr and 5mg Salbutamol neb)
- Coagulation screen – only if on anticoagulant or abnormality likely
- ECG if history of IHD, glucose if diabetic
Observations
- Record BP – postpone only if very high
- Assess and document peripheral pulses
Fluid management
Ensure patient well hydrated and good urine output prior to contrast (if pre-dialysis) – if in doubt put up 6hrly 500mls N Saline. Do not fluid overload dialysis patients. Avoid diuretics. Beware that after stenting/angioplasty, some patients may become polyuric.
Consent
Should be done in OPD for diagnostic studies. Radiologist should obtain consent for interventional studies, need to warn of risks of contrast, and catheter-related complications including embolism, arterial occlusion, bleeding from puncture site, loss of renal function, occasional need for surgery after intervention.
Post-procedure
- Diagnostic studies – mobilise at 4 hours if no complications
- Interventions – mobilise at 6 hours, and overnight stay
- Pulse and BP – hourly for 4 hours, then 6 hourly overnight if IP
- Urine output – beware polyuria post-angioplasty
- Assess pain, wound, haematuria
- Check U&E following morning if kept in
- Warfarin can be restarted the following day
- Consider Aspirin 150mg if angioplasty/stent – ask radiologist if not clear
Angiography and angioplasty – information for patients from EdRenINFO
Myeloma skeletal survey
(In Edinburgh, request in these words) – includes CXR, lateral skull, lumbar spine, pelvis, upper femur; plus 2 views of any symptomatic region.
Ultrasound
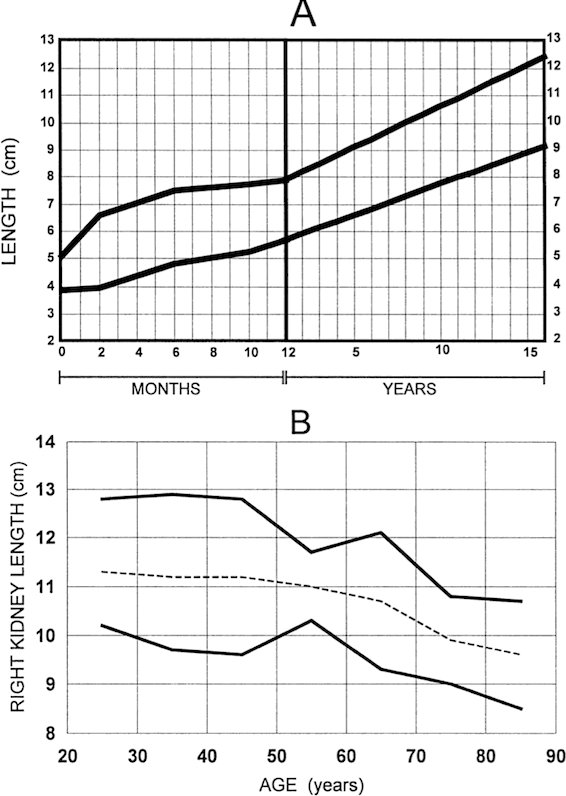
The most requested and most frequently useful investigation, but observer dependent – speak to the operator if any question. Renal length averages 11 cm in adults, but there is some variability in measurement, and differences of up to 1cm in repeated measurements are common. Figures showing 95th centiles are from O’Neill, Am.J.Kid.Dis. 35:1021-38 (2000).
Contrast nephropathy
This is probably rare, but occasionally real. The risk of it has been exaggerated, and most studies of it weakened, by using surrogate endpoints such as small rises in Creatinine, rather than real events such as oliguria, need for dialysis, or lasting change in renal function. Many of those receiving contrast have alternative explanations for AKI (therefore contrast-associated, rather than contrast-induced AKI).
Risk factors:
- Under-hydration/hypovolaemia
- Myeloma
- Renal impairment
Prevention
Contrast type and dose: the use of lower doses and probably less hyper-osmolar contrast media are thought to reduce risk.
Prevention: Testing of almost all putative protective treatments has shown them to be harmful – this includes marnnitol, diuretics, and dopamine; or of no benefit (N-Acetyl Cysteine; hydration with bicarbonate rather than saline).
Pragmatic approach: If a patient is at significantly increased risk, does this alter the balance of risk for doing/not doing the test? If not:
- Warn the patient
- Withhold diuretics
- Ensure adequately hydrated. If supplementary IV fluid required, N saline is as effective as bicarbonate solutions. Be careful not to overload with salt. Avoid diuretics. 6hrly 500mls N Saline once will generally be safe if you feel that oral hydration and omitting diuretics is not enough. There isn’t a particular IV fluid regimen to recommend that would be applicable and yet safe for all patients in these circumstances.
Acknowledgements: Angela Webster was the original author for this page. Contrast nephropathy section rewritten by Htet Khin, April 2020. The last modified date is shown in the footer.