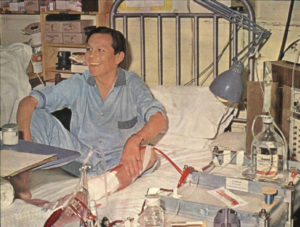
Robin Eady on dialysis at the Royal Free Hospital in 1966
Robin Eady was one of the very early patients treated by dialysis for chronic renal failure, a diagnosis made while he was a medical student. In this 2001 British Journal of Renal Medicine interview, ‘The dawn of dialysis – reminiscences of a patient’ he describes his early experiences undergoing pioneering haemodialysis treatment in the early 1960s and subsequently transferring to London. He later graduated, became an academic dermatologist, and later Professor of Dermatology.
The text is reproduced by kind permission of the author and of Hayward Medical Communications, publisher of the BJRM.
When did you discover you had a problem with your kidneys?
Discovering that proteinuria can matter
I was nine years old. A routine medical check-up at school showed that I had protein in my urine. After extensive testing in hospital, it was thought that the proteinuria was related to my posture, and not caused by a kidney disorder. My parents and I were told there was nothing to worry about.
When did things get worse?
I was playing in a vigorous game of hockey while a medical student at Guy’s. Suddenly, I felt a severe crushing sensation in my chest, was short of breath and had tingling in my fingers and lips. I had just started my clinical studies, and with my newly found knowledge, suspected I’d had a heart attack. The symptoms passed, and I returned home exhausted. Over the next few weeks I had severe, unrelenting, pounding headaches and often felt sick. I felt worse after drinking beer, which was a sort of staple food for students then, as it possibly is now. I asked a fellow student to take my blood pressure, and he found it to be sky high. Neither he nor I believed the readings, but rechecking confirmed the result. I was admitted to a medical ward at Guy’s almost immediately, and learned for the first time that I was suffering from kidney failure. The initial diagnosis was ‘acute nephritis’. The hypertension had strained my heart and kidneys, so control of my blood pressure was given the highest priority.
What happened next?
Treatment for renal failure without dialysis
The medicines used to treat my hypertension had severe side-effects, and I began to think that the cure was worse than the complaint. The marked swings in my blood pressure caused repeated fainting sensations associated with alarming palpitations. Consequently, I had to spend two hours in the morning getting up, washed and dressed. Another, almost intolerable, burden was the imposition of a rigid diet, with drastic restrictions imposed, especially in my intake of protein and potassium. My daily allowance was 20 g of protein, the equivalent of one egg, or a tiny portion of meat or fish. Vegetables, including potatoes, had to be boiled to the extent that they became mushy and unappetising. I felt ghastly – this was the start of the lowest period in my life. More about the treatment of chronic renal failure before dialysis.
How long did you remain in hospital?
Not long. My parents were informed that the outlook was very gloomy. My older sister had died in a plane crash a few years previously and it seemed that they were soon to lose their only surviving child. A family friend, who was also a doctor, made arrangements for me to consult a leading kidney specialist at another London teaching hospital. Kidney specialists were hard to come by, and nephrology was not yet recognised as a sub-specialty in British medicine. Further tests showed irreparable kidney failure. The only line of treatment that was available was based on damage limitation: the same diet, a variation of the same medicines and repeated blood transfusions. The transfusions were for the severe anaemia that accompanies renal failure.
Did you ever feel like giving up?
Curiously, no. I had an intense desire to live, although, in many ways, there was no semblance between my lifestyle and that considered normal for a man of my age (I was then 21). As described earlier, the relatively simple act of getting up in the morning expended most of my limited energy. This was a tremendous change from my previous lifestyle. My early days as a medical student were among the best of my life. I had been part of a close-knit community, studying and playing sports with my fellow students. I managed to return to my studies part-time, but had absolutely no social life, and after a few months, I gave up the struggle to keep up my studies and returned home to live with my parents. This, in itself, was strange because until I entered Guy’s I had been at boarding school from the age of nine, and had only been home during the holidays. My parents lived abroad, so short weekend visits were not an option then. Home life always had a beginning and an end, and was normally limited to one or two months at a time. My parents were enormously supportive and worked hard to maintain my optimism (cheerfulness would have been unrealistic). As a family, we never gave up hoping that there would eventually be an effective treatment for my rapidly declining health.
How did you hear about dialysis?
Dialysis for chronic renal failure in Seattle
Never underestimate the power of the popular press! During a visit to the hairdressers, my mother read in Life magazine about a revolutionary new way of treating patients like myself. Almost simultaneously, my father’s attention was drawn to a piece in the French periodical, Paris Match, covering the same story. The new treatment was called haemodialysis, and was a method of cleansing the blood of toxins and waste products that had accumulated in the body as a result of the kidneys ceasing to function normally. Up until that time, haemodialysis had been used only in a few centres in North America and Europe, and only as a treatment for acute, and short-lasting renal failure.
It was a major undertaking and was only used for treating patients with what was thought to be a reversible crisis. The few patients who had benefited required several dialysis treatments to tide them over until their kidney function picked up again; a process that usually took only a few days or weeks. There were several reasons why the treatment would not be suitable for patients with irreversible kidney failure.
The new approach, introduced by Dr Belding Scribner and his colleagues at the University of Washington, Seattle, USA, enabled the treatment to be repeated over months or, as had been found in the first pioneer patients, years. This was made possible by the development of a novel device, later known as the ‘Scribner Shunt’, for providing repeated access to the patients bloodstream. This invention is now recognised as a turning point in modern medical history. More on the shunt
Who benefited from the new therapy?
As places on the early programmes were severely restricted, it was necessary to select who would and would not be eligible for treatment. These difficult decisions were made by a committee whose members were drawn from the church, medical profession, law and lay public. The formation of such a committee was, in itself, apparently novel, and certainly newsworthy. The implications were self-evident: the committee literally had the power of life and death.
Did haemodialysis seem to be the best option for you at the time?
Indeed it did. Renal transplantation was still experimental, and had only been successful when the donor and recipient were identical twins. My mother and uncle had been assessed as potential donors, and found to be unsuitable. Thank goodness!
How did you manage to get on to the Seattle programme?
Not because of any encouragement from my doctors in London, with the exception of a senior registrar, who is now a distinguished professor [Professor Sir Colin Dollery; personal communication Robin Eady]. My consultant solemnly told me that I would be wasting my time, and my parents money, if I went to Seattle.
It was at the end of 1962, and I had just had my 22nd birthday. Fortunately, my father’s persistence, and the intercession of a family friend in Seattle, whom I didn’t know at the time, somehow (nobody quite knows how) persuaded Dr Scribner to offer me a place. But his offer was conditional, for reasons I’ll describe later. I left London for Seattle, accompanied by my parents, in February 1963. I had to be carried onto the plane at Heathrow, because of my general debility and extreme weakness. The Boeing 707 flew us non-stop across the newly-introduced polar route.
Can you remember being prepared for your first dialysis?
The Scribner shunt and first dialyses
First, the cannulas (small plastic tubes) were inserted into an artery and a vein in my left forearm. The external parts of the cannulas were joined together with a U-shaped tube; this last component was known as the shunt. The cannulas were made of two types of plastic, Teflon and Silastic which, unlike glass and other plastics, had special properties that prevented or slowed clot- ting on contact with blood. More on the shunt
The insertion of the cannulas, performed under anaesthesia, took several hours. The surgeon had to be satisfied that the blood flow was adequate and that the delicate inner lining of the blood vessels was protected from any undue damage caused by movement of the cannula tips. The cannulas were stabilised both under and outside the skin. We were taught to take great care of our cannulas, which involved daily cleaning, and the application of a protective dressing. Regular checking of the shunt was necessary, looking specifically for evidence of clotting or for loosening of the connections with the cannulas. If the blood flow was inadequate, clotting was inevitable. This could occur at any time, and was always treated as an emergency. The removal of the clots was usually painful, and was always nerve-racking for the patient, and stressful for the medical and nursing staff. If it failed, dialysis was impossible without revision of the cannulas. With luck, the arterial cannula might survive a year or so without revision, whereas the venous cannulas needed replacing more often.
What was your first dialysis like?
I was in a room with three other patients, two men and one woman, who were the original pioneers in the Seattle programme. One of them was Clyde, who has often featured in articles describing those early, historical events. At that point, Clyde had been on dialysis for two years, the longest period for that time. Although still quite young (he was aged about 43, if my memory is correct), he was a sort of father figure to a new boy such as myself.
The second patient, Harvey, was younger and generally less tolerant. His rebellious character had probably helped him to cope with the many deprivations associated with his new, constrained lifestyle. He was a father of young children and a part-time shoe salesman. Before long, Harvey asked me, ‘Where did you get those terrible shoes; was it in England?’ I had to admit that the bright tan colour of my British brogues was not to everyone’s taste. I took Harvey’s tip and ditched the shoes immediately, and bought my first pair of American sneakers.
The third patient, Cathy, was older than myself, always friendly, and was, I think, curious about the young man who had recently arrived from England. Occasionally, there was a fourth patient, Rolin, who arrived in a wheelchair and had to be carried to the bed. He was skin and bone and suffered with a severe neuropathy as a result of his renal disease, which had remained untreated for too long before he started dialysis. The first dialysis lasted only a few hours, but the routine then became two 12-hour dialyses every week. The treatment took all day, and sometimes ran into the night.
How did you feel during dialysis?
Although the equipment in use then would seem like a museum piece now (I believe some of it has actually been donated to a museum), it performed very effectively. The main difference between it and the equipment used today relates largely to the newer methods used for accessing the patients bloodstream and the availability of disposable, and highly efficient, dialysers. As a consequence of these improvements, the treatment period has been drastically reduced. There were occasional technical hitches, but I can recall only one that was potentially dangerous. Owing to a build-up of a high pressure of dialysis fluid in the system, my blood was forced backwards through the artery in my arm and up to my brain. I experienced a fleeting moment of double vision and partial loss of consciousness. Fortunately, the symptoms didn’t last. The next day, the neurologists asked me to appear at grand rounds, the weekly doctors’ meeting, because they thought my case was worth discussing as a medical novelty. (Ironically, exactly 35 years later, I was invited back to Seattle to deliver a prestigious guest lecture, and conduct grand rounds myself.)
How long did it take before you felt well?
About four to six weeks. I was still very weak, but gradually regained my strength. For the first time, there was a strong emphasis on restricting my intake of salt and fluid. My blood pressure returned to near-normal levels quite rapidly, and it was a great relief to stop taking the blood pressure tablets, whose side-effects had been hard to tolerate.
How long did you stay in Seattle?
Becoming a renal technician
For only four months. One has to remember that dialysis was available to only a very few patients, and the facilities could not meet the demand, even from those needing it in the local population. Dr Scribner had arranged with Dr Lionel McLeod, then in charge of the renal service in the University of Edmonton, Alberta, Canada, that I would receive training as a renal technician in Seattle. Then, when I was fit enough, I would move to Edmonton, where I would work in the new Artificial Kidney Laboratory. I would continue to receive dialysis in Edmonton until the treatment became available in England.
What did the technical training entail?
Nothing came pre-packed or sterilised. The various chemicals required for making the dialysis fluid had to be individually weighed and packed. I was taught to mould the fine Teflon tubing into the U-shaped shunts to fit the needs of each patient. The Seattle water was very soft, and I believe we used it straight from the mains supply. The was no water treatment, apart from simple filtration.
Doubtless this practice was later modified. The preparation of the Kiil dialysers, or ‘kidneys’, required the greatest skill. These consisted of a stack of three heavy slabs, or boards, of polypropylene, enclosing two layers of cellophane sheets that acted as dialysis membranes. These sheets were soaked in a sterilising solution and, while still wet, were applied in pairs over the grooved surfaces of the boards. (More about Kiil dialysers at home; and Kiil dialysers in Edinburgh.)
This two-person task was technically very demanding because of the need to avoid trapping air between the two sheets, or between the cellophane and the boards. After the first stack had been made, the procedure was repeated so that the finished product resembled a double-decker sandwich that had been fastened together with large industrial bolts.
Then came the tricky part. The kidney had to be tested for leaks, by pumping air in between the membranes and noting any drop in pressure over a minute or two. If the pressure test failed, the whole process of stripping and assembling the kidney had to be repeated. Even skilled technicians might be expected to take half an hour to complete the job. Just imagine the strain this could inflict on couples having to do this for themselves at home.
You said that you then moved to Edmonton?
To Edmonton, Canada, until treatment in Britain was possible
Yes, when I was back on my feet and had received the rather basic training as a technician, my parents and I moved to Canada. My father had retired, and I was fortunate that he and my mother were able to support me in such a comprehensive way. I continued to be treated in the University Hospital in Edmonton. I was again privileged to be included among the first Canadians to receive chronic dialysis. Another patient, Jim, never removed his cowboy boots and smoked his own-rolled cigarettes throughout the treatment period. The second patient, a teenage girl, was probably the youngest patient in the world at the time. We spent many hours in each others company, often watching ‘The Dick Van Dyke Show’, and other, more mindless television programmes, characteristic of the early 1960s.
What was it like to get back to work?
I wasn’t much good as a technician, but my colleagues were very generous. My lack of success was partly due to the fact that I found it psychologically difficult to work so close to my lifeline, and because I really wanted to return to my medical studies. Dr McLeod understood how I felt and arranged for me to attend lectures in the University of Alberta Medical School, in Edmonton. I also assisted a young postdoctoral scientist with his neurophysiology experiments. I was thus able to cut my teeth in scientific research, albeit in a peripheral capacity. This early experience has probably helped in steering me into a career in academic medicine.
How long did you remain in Canada?
Home to dialysis in London, 1964
Eighteen months later, 1964 saw the development of two dialysis programmes in London. One was headed by Professor Hugh DeWardener at the, then new, Charing Cross Hospital (Fulham branch), while the second was run by Stanley Shaldon at the Royal Free Hospital, in Hampstead. Naturally, I got in touch with both of these doctors and each responded encouragingly about the possibility of my becoming their patient upon my return to the UK. I had the opportunity of meeting Dr Shaldon during his visit to Edmonton, and decided to accept his offer. I returned to London in December 1964.
At the time, I had no means of knowing that within four years I would have married, qualified in medicine and completed my first year’s work as a junior doctor. How could anyone have predicted that, with my new wife’s help, I would also have set up dialysis in my own home? Those were indeed remarkable times! In 1965 The Evening News published a group photograph of the dialysis patients at the Royal Free, in which they described us as The Lucky Thirteen. But sadly, none of the other 12 patients or any of the other pioneers I came to know and respect in Seattle and Edmonton is alive today.

The ‘lucky 13’ first chronic haemodialysis patients at the Royal Free Hospital under the care of Dr Stanley Shaldon on Janurary 1st 1965. Robin Eady is identified second from right on the front row by the arrow. More on home haemodialysis
When a life-threatening illness strikes someone out of the blue, the natural reaction is to ask, ‘Why me?’ I now find myself asking this question again. But this time I ask it after living through an extraordinary period in the history of renal medicine. Perhaps it would be better if I didn’t try to seek answers, and accepted my lot graciously.
I would like to dedicate this short article to the memory of my fellow patients in Seattle, Edmonton and London. Their friendship and courage has helped me in ways that are difficult to describe. Robin Eady.
Further reading
Dr Belding Scribner, founder of dialysis for chronic renal failure in Seattle, wrote a 60th birthday tribute to Robin Eady, by then the longest surviving dialysis patient in the world, in 2000. (Also paywalled from Haemodialysis International).
The skin disease charity DEBRA posted an obituary about Professor Eady’s academic research into epidermolyis bullosa, and his training of future dermatologists.
